Having a functional medical problem like Irritable Bowel Syndrome (IBS) suggests that there is a level of activation acting on your Autonomic Nervous System (ANS) that is outside of your “window of tolerance”. In this blog post, I’m going to be addressing the concept of the window of tolerance and why it’s important for healing from a functional gastrointestinal problem.
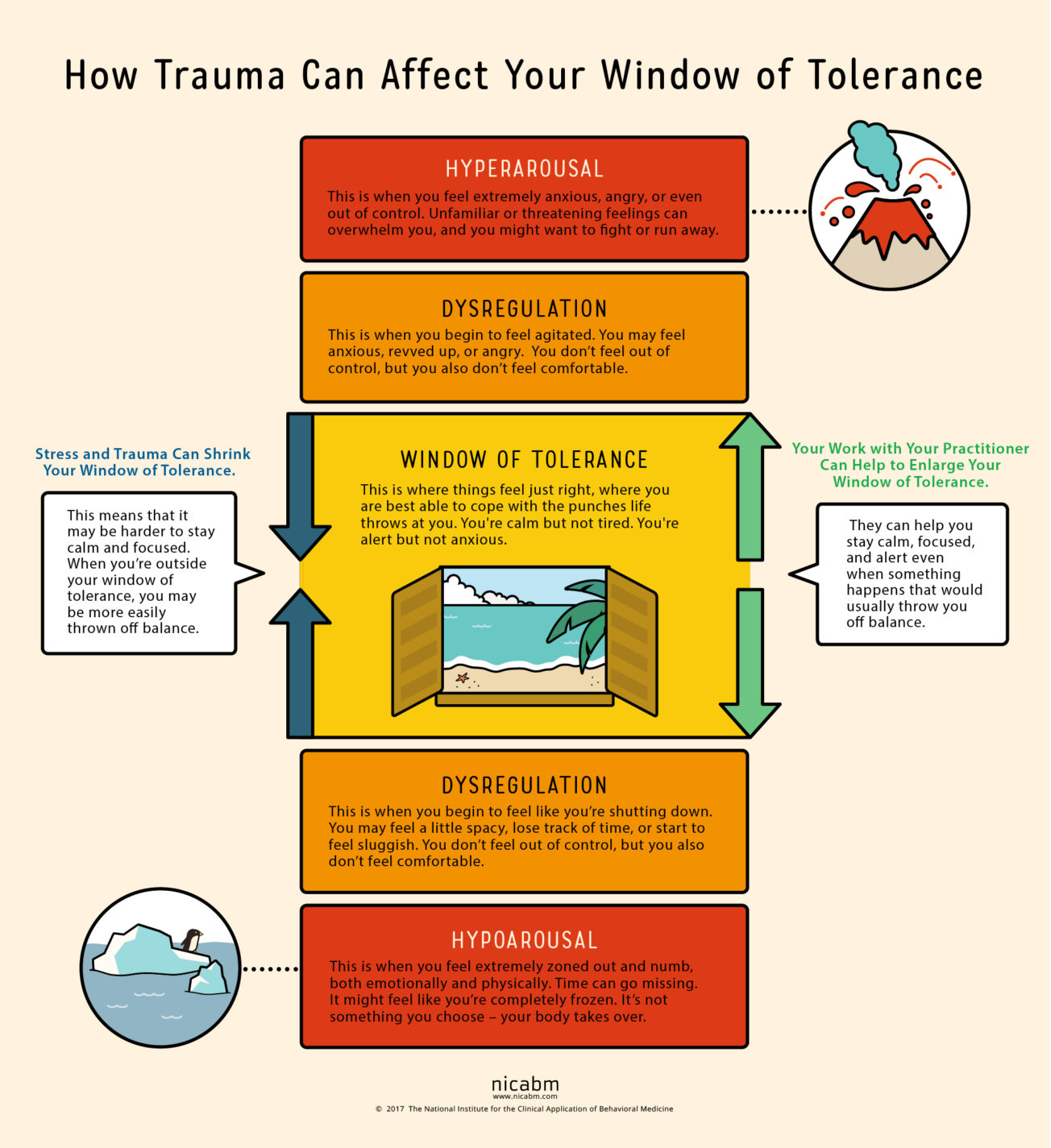
Window of Tolerance
The term “window of tolerance” was coined by a well-known UCLA neurobiologist named Daniel Siegel, M.D. Siegel has been involved in the ever-growing research on the effects of mindfulness meditation on the brain and has written many books on the benefits of mindfulness. If you ever have a chance to hear him speak, go. Siegel is an incredibly engaging speaker, making learning about our own neurobiology fun. If you feel like picking up one of his books, try reading The Mindful Brain.
Everyone has a window of tolerance. Your window of tolerance refers to how much stress your body can manage without being overwhelmed or without your parasympathetic nervous system generating a freeze, shut down, or dissociative response. Interestingly, flare-ups of functional gastrointestinal symptoms are often not mentioned in the list of symptoms that occur when stress exceeds the body’s ability to manage it, but they certainly should be. You probably notice the cyclical nature of your functional medical symptoms. Some, most, or all of the coming and going of functional medical symptoms is likely attributable to your body’s inability to manage effectively the level of stress it is under, or in other words moving outside of your window of tolerance.
Traumatic experiences are extraordinarily stressful events. We all face traumatic experiences in our lives in some form or another. Trauma can have a huge impact on our windows of tolerance. More on this in a future blog post. For now, suffice it to say that stress and trauma are linked to functional medical, especially gastrointestinal, problems,
Surpassing Your Window of Tolerance Generates Functional GI Symptoms
(For Those Prone to Having Functional GI Disorders like IBS)
When you get really nervous before going on stage to perform or giving a speech in front of a large group of people and your stomach is in knots, that is a sign of stress being higher than normal. We know that the body is affected by stress. We know that gastrointestinal symptoms can easily result from stress. Getting nervous knots is a prime example. Most likely, if you have nervous knots in reaction to a clear stressor, then you are within your window of tolerance. When GI symptoms get more intense, more painful, or more debilitating than nervous knots, then we could say you are outside of your window of tolerance.
Functional GI symptoms like Irritable Bowel Syndrome symptoms are similar to nervous knots in that the ANS is generating some kind of stress response that results in belly sensations. The differences are the intensity level, the chronicity, the stressor(s), and your level of awareness.
Functional GI symptoms like abdominal pain are much more intense than nervous knots, and they don’t necessarily go away quickly. And even when they do go away, they come back. Functional GI symptoms often happen seemingly for no reason (seemingly no stressor) at times when things may seem relatively okay. You may not even recognize that you feel any more stressed than you have in the days leading up to the GI symptoms.
Easy to Exceed Your Window of Tolerance If You Don’t Recognize Stress
In my personal and professional experience, many people with GI symptoms don’t realize just how much stress or anxiety, which is really a form of ongoing stress, their bodies are under. In other words, they live day to day towards the top or bottom of their window of tolerance without knowing it. If you are living towards the top or bottom of your window of tolerance, it doesn’t take much more stress for you to get bumped out of your window. When that happens, your body is likely to generate symptoms of IBS or GI dysfunction.
I suspect that GI dysfunction is not mentioned as part of the symptom experience arising from moving outside of the Window of Tolerance because stress and the stressor are often not recognizable at the time one experiences the GI distress. Why would anyone say that they are suffering from stress without feeling that their body is under stress and without being able to identify a clear stressor? They wouldn’t. Nor should you.
However, just because you don’t recognize that your body is experiencing stress doesn’t mean stress is not a factor in your GI symptoms. Similarly, assuming you do recognize that your body is experiencing stress, just because you aren’t able to identify a clear stressor doesn’t mean that the stress has no reason to exist or is somehow invalid.
Your window of tolerance is not what you think you can handle; it’s what your body can actually handle. What you think you can handle is what the conscious, rational, analytical part of your brain thinks, not what your ANS experiences.
Promote Healing by Learning About Your Own Window of Tolerance
Part of healing from a functional GI disorder like IBS is recognizing that what you think or believe right now about your body’s experience of stress and your body’s capacity to manage stress effectively may not match up to what your body actually experiences in reaction to various stimuli. Your Autonomic Nervous System does not do what it wants you to do; it does what it already knows how to do, and it doesn’t need your approval or even awareness to do it.
Don’t let what you think you know get in the way of discovering what you actually need to know in order to heal your body. Do the inner work necessary to heal from whatever kind of functional gastrointestinal problem you are dealing with, be it IBS, cyclic vomiting, chronic pain/dyspepsia:
• Take time—weeks or months—to learn about your ANS. Try to be curious and open to discovering what your ANS does in all kinds of different situations with all different kinds of people in your life.
• Try to become more aware of what you think, believe, and assume about the way your ANS and body do stress.
• Seek to discover what your ANS is actually doing by slowing down and paying attention to yourself in ways that you may not otherwise be paying attention to.
• Cultivate greater self-awareness and mindfulness skills. Incorporate the skills you need most into your day-to-day life, paying attention to your body’s reactions to things that occur.
• Once you have enough data, use this information to modify your behavior in small ways that you believe will make a difference in how you reduce and manage stress.

0 Comments